What Is Spondylolisthesis?
Lumbar spondylolisthesis is a medical condition affecting the spine, characterized by the displacement of one vertebra relative to the adjacent vertebra. The term derives from Greek, where “spondylo” means vertebra and “listhesis” implies slipping or displacement. This disorder can occur due to degenerative causes or from a fracture of the junction between vertebral joints, known as lytic or isthmic spondylolisthesis.
Lytic or Isthmic Lumbar Spondylolisthesis: Causes and Symptoms
Lytic spondylolisthesis occurs due to a fracture in the pars interarticularis, the portion of the vertebra that connects the facet joints to each other. This fracture can result from minor trauma in patients who already have a predisposition to weakness in this structure. While not a congenital condition per se, weakness of the pars may be present from birth. Symptoms can range from mild pain to severe sciatica, depending on the degree of displacement and nerve involvement. This Spine Health article provides an illustrative 3D video reconstruction of this condition.
The displacement of vertebrae relative to each other causes progressive narrowing of the neural foramen, potentially compromising the exiting nerve root—a finding closely related to the grading of this pathology.

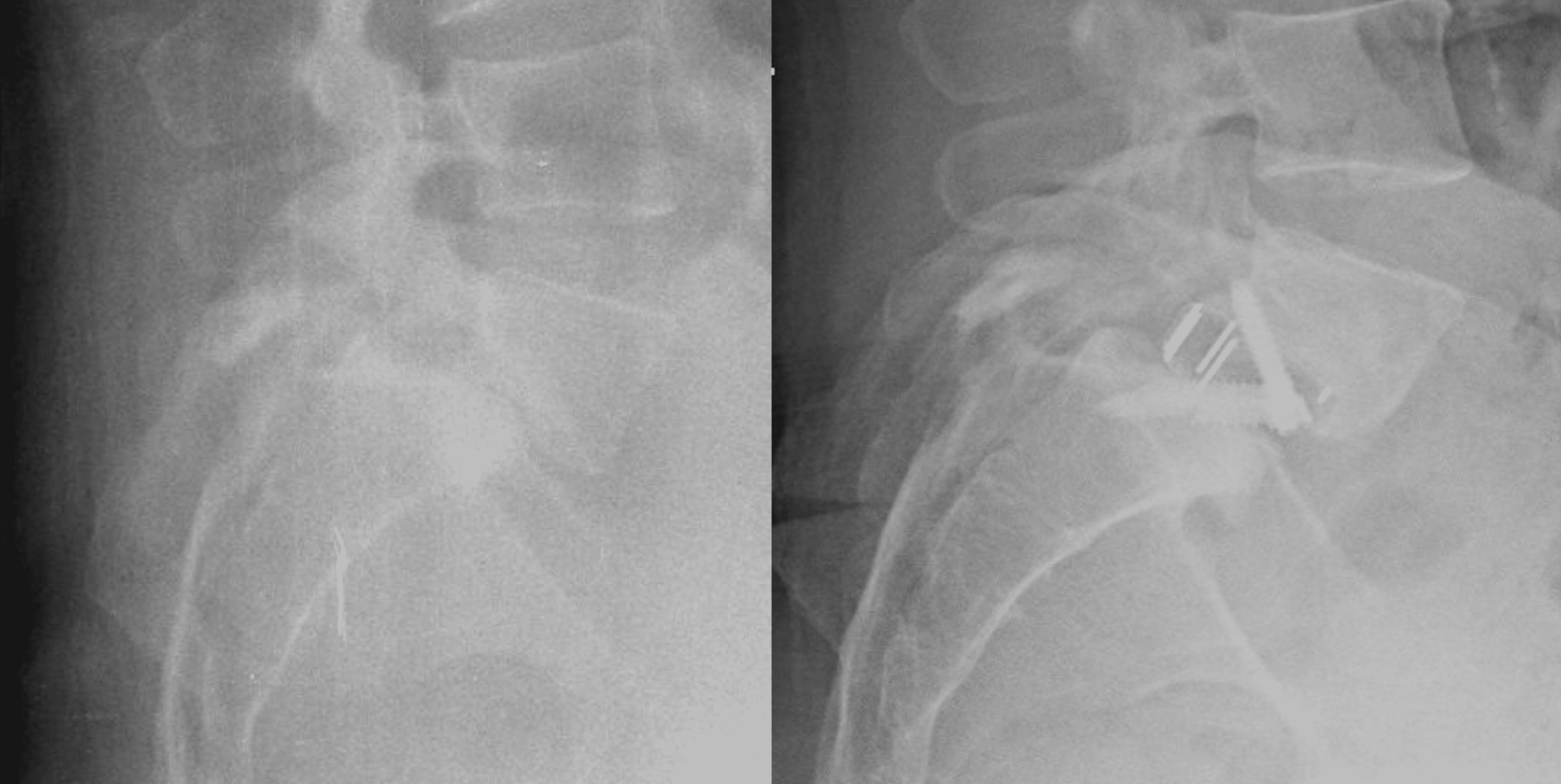
For descriptive purposes, spondylolisthesis—particularly the lytic type—is classified into grades based on the displacement of the affected vertebra relative to its neighbor. Displacement of up to 25% is considered Grade 1, 25-50% Grade 2, and so forth up to Grade 5 or spondyloptosis, a rare condition in which the upper vertebra falls anterior to its lower adjacent vertebra. The severity of displacement does not correlate with symptom severity. In fact, some advanced cases of spondylolisthesis may be discovered incidentally during X-rays performed for other reasons and remain permanently stable and asymptomatic at diagnosis. However, grading information can be relevant when planning potential surgery.

Degenerative Lumbar Spondylolisthesis: Factors and Manifestations
Degenerative spondylolisthesis, on the other hand, develops due to wear and tear of the vertebrae and intervertebral discs, particularly in women. This degenerative process leads to instability in the lumbar segment, particularly at the L4-L5 level. Misalignment between vertebrae can cause chronic low back pain as well as symptoms of nerve compression such as sciatica.

When Should Surgery Be Considered?
The decision to surgically intervene in cases of lumbar spondylolisthesis depends largely on symptoms and the progression of the condition. While some patients can live with spondylolisthesis without experiencing significant discomfort, others may require surgical treatment to relieve pain and prevent future complications. Surgery is typically considered when there are debilitating symptoms, progression of vertebral displacement, or nerve compression.
Considerations for Surgical Treatment
Surgical management of spondylolisthesis, especially the lytic variety, is demanding and requires an experienced surgeon due to the significant structural changes affecting anatomical elements that constitute a pathology-specific anatomy not easily recognized until sufficient experience has been accumulated. The surgical technique must be definitive on the first attempt, as risks associated with additional procedures can be significantly higher than in virgin tissue. In cases of degenerative spondylolisthesis, treatment is similar to other degenerative spinal conditions, focusing on stabilization and decompression of the affected segment.
In summary, spondylolisthesis is a complex condition that can have a significant impact on patients’ quality of life. Understanding the causes, symptoms, and treatment options is the key to therapeutic success.
If you would like a second opinion regarding your spine condition or treatment plan, please contact our team.